Venous Stasis Ulcers
What is a Venous Stasis Ulcer?
Venous stasis ulcers are hard-to-heal wounds that are common in people with vein conditions. People with venous stasis ulcers should seek specialized care with a physician in a timely manner to prevent complications like infections that can lead to amputation or become life-threatening. These ulcers are known to heal and come back if prevention is not part of consistent and preventive care. Compression therapy is an important treatment for preventing ulcers from reopening.
How is a Venous Stasis Ulcer Diagnosed?
A venous ulcer can typically be diagnosed through a physical examination, and there may even be testing performed. The healthcare provider will gather additional health history information regarding potential factors and risks associated with underlying conditions that could have contributed to the development of the ulcer.
How Do Venous Stasis Ulcers Develop?
Insufficient blood flow in the leg veins is what causes venous stasis ulcers. Chronic venous insufficiency frequently causes valve dysfunction. It happens when your valves malfunction or don’t have enough strength to do their job. Valves within the veins of the legs regulate blood flow. However, these valves can become damaged and compromised, resulting in altered blood flow and the development of ulcers. Without sufficient blood flow, the body has difficulty healing, causing ulcers to persist.
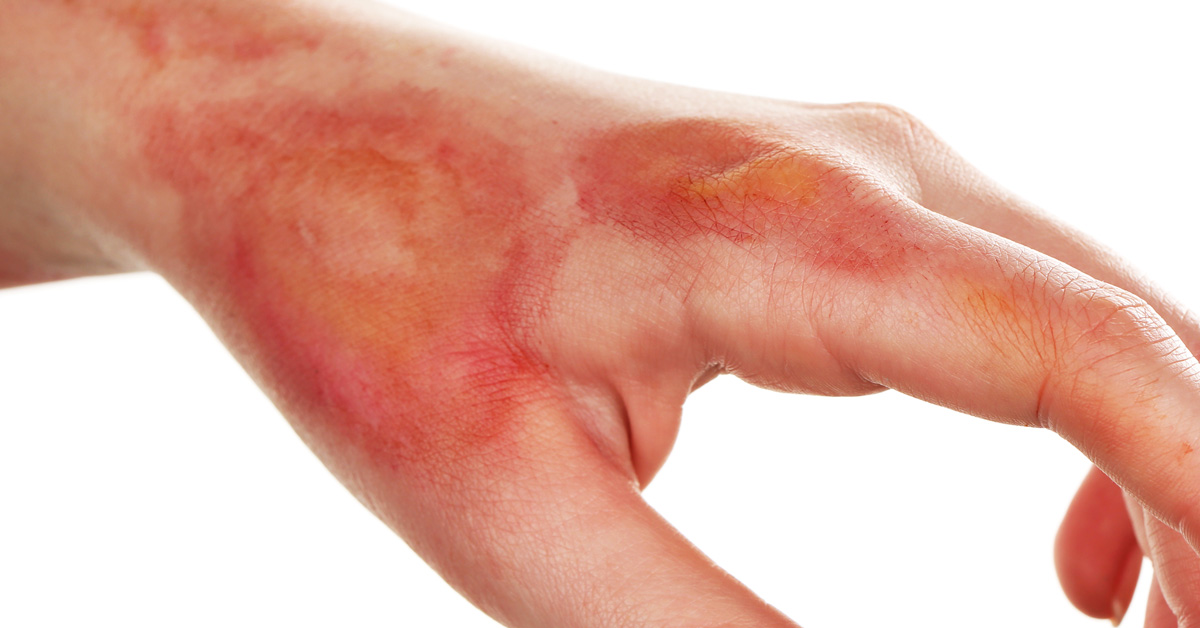
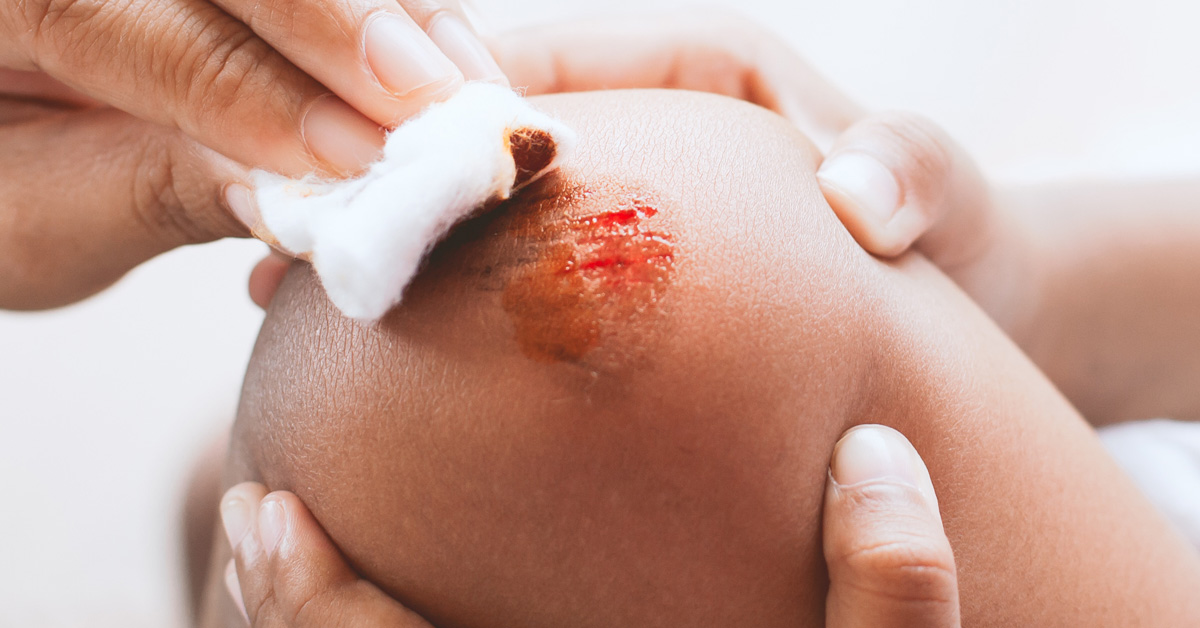
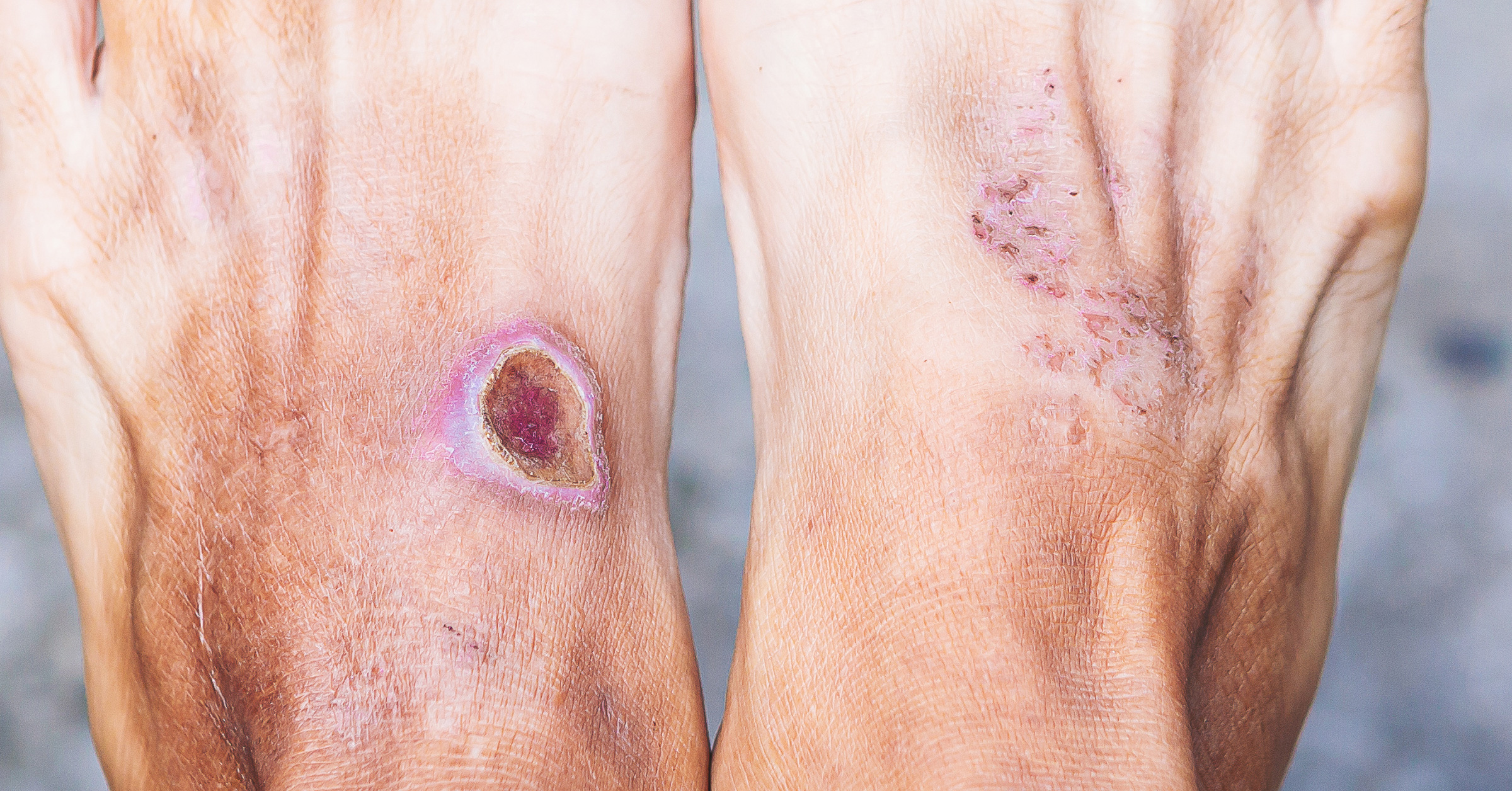
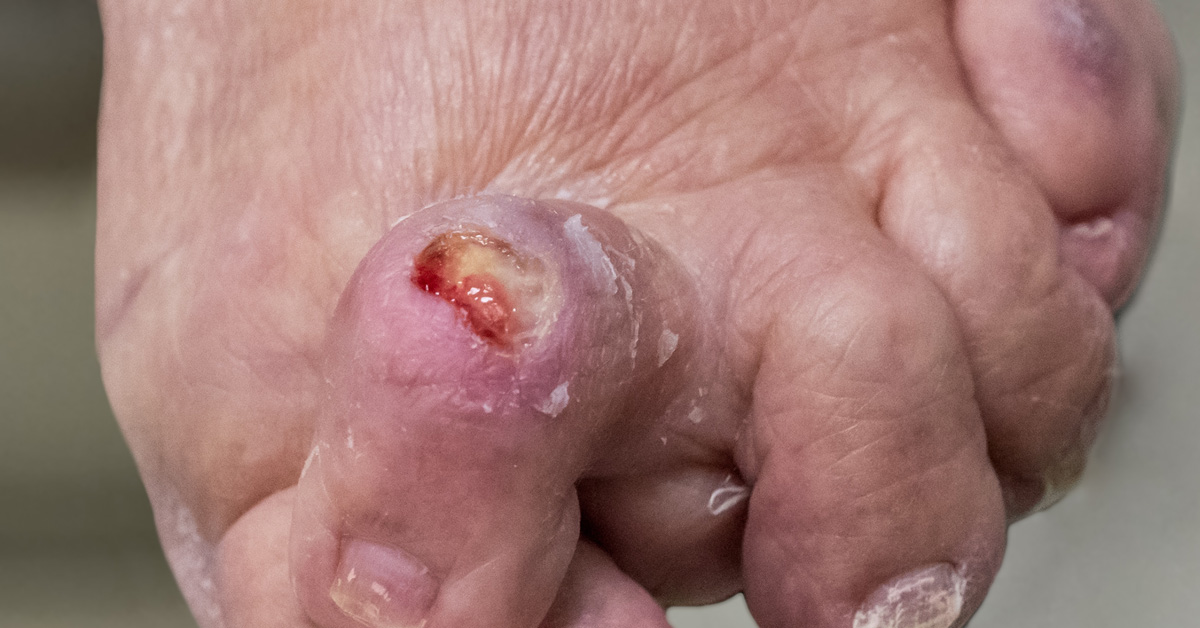
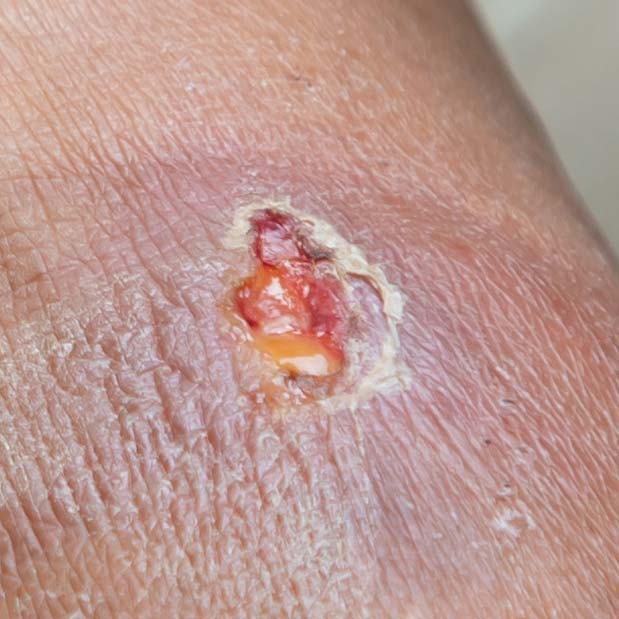
What Do Venous Stasis Ulcers Look Like?
They are typically shallow ulcers that are irregularly shaped. The skin around the stasis ulcer may become discolored and firm. The symptoms may include:
- Leg swelling
- Fluid that drains from the ulcer
- Itching
- Dull ache
- Foul odor from drainage
Who is at Risk for a Venous Stasis Ulcer?
There are a variety of risk factors that can cause venous stasis ulcers. These conditions can include:
- Obesity
- Aging
- Paralysis and sedentary lifestyle
- Family history of venous stasis ulcers or disease
- Varicose veins, spider veins, and deep vein thrombosis
- Smoking, alcoholism
Why is it Important to See a Doctor?
Venous ulcers need consistent help to heal. The longer you live with a venous stasis ulcer, the more likely it is that permanent tissue damage will occur. The damage can spread or cause infections that are potentially fatal. This risk is significantly reduced when wound care is received on time from an experienced wound care provider.
How Can I Prevent Venous Stasis Ulcers?
If someone has previously experienced an ulcer, following these steps can reduce the likelihood of an ulcer recurrence subsequent to treatment.
- If you smoke, quit. Take part in a smoking cessation program.
- Eat a healthy diet while maintaining a healthy weight.
- Follow your doctor’s instructions for any chronic conditions you may have, like diabetes or high blood pressure. These affect vein health.
- Keep your legs elevated above your heart while sitting.
- Stay active with exercise, like walking.
- If your doctor has prescribed compression stockings or clothing, wear them.
Why Did my Doctor Order Compression Therapy?
Compression therapy is often ordered to improve blood circulation in the lower legs. This therapy helps with pain and swelling (edema) in the legs. Elastic stockings, compression garments, compression wraps, and inflatable devices are examples of effective compression therapy. Wearing compression therapy ordered by your physician will help keep blood from pooling in your legs, ankles, and feet. The blood needs help to flow upward toward the heart.
How To Treat Venous Stasis Ulcers at Home
- Wash your hands to prevent infections.
- Cleanse the wound with AMERIGEL® Saline Wound Wash before every dressing change.
- Apply a layer of AMERIGEL Hydrogel Wound Dressing with a gloved finger or tongue. This dressing is appropriate for venous leg ulcers, as directed by your doctor.
- Cover your wound with an absorbent bandage, like an AMERX® Bordered Gauze Dressing. Your wound should be covered in order to heal properly. Wounds that are exposed to air heal more slowly because the surface cells dry out, and as a result, they are more susceptible to infection.
- Change your wound dressing daily, repeating steps until it heals.
NOTE: If you are experiencing any symptoms suggestive of a medical emergency, always contact a physician or seek urgent care immediately.